Balanoposthitis – Treatment, Pictures, Symptoms and Causes
What is Balanoposthitis?
Balanoposthitis is a condition seen in uncircumcised males where the glans penis and the prepuce are inflamed due to several infections related to the non-removal of the foreskin. This is frequently due to unretractility of the foreskin and very poor personal hygiene, which results to too much bacterial and fungal growth around the area. This condition is only exclusive to males. Most of the affected group comes from children 0-5 years old and in adult males who actively engage in sexual intercourse. Other medical conditions may also precipitate to balanoposthitis, which can be more severe. This can become the point of onset of bacteraemia and fever in men with very low levels of neutrophils. Patients with diabetes mellitus are also susceptible to candidal balanitis. This can also become an entry way for acquiring infections. Morbidity of this condition is only limited to its associated symptoms. Death is at hand only to those patients who are immunocompromised and those who develop balanoposthitis consequential to septicaemia caused by fungi. Intermittent balanoposthitis caused by candida albicans results to mondor phlebitis. Severe balanoposthitis enhance the probability of balanitis xerotica obliterans, tightening of the foreskin or phimosis, cancer and paraphimosis.
Balanoposthitis Symptoms, Signs
Upon physical examination, the following signs and symptoms can be noted:
- Red, damp unelevated lesion on the glans and foreskin
- Soreness
- Irritation
- Redness of the penis
- Painful penis and prepuce
- Rashes around the penis
- Presence of discharge beneath the prepuce
- Tightening of the foreskin or phimosis
- Foul smelling discharge
- Apparent ulcerations
- Unusual enlargement of the lymph nodes over the groin area
- Fatige
- Low back pain
- Anxiety
Balanoposthitis Causes
In nearly all cases of balanoposthitis results from the existence of the foreskin or prepuce, which may be unnecessary and tightened, making it more susceptible to different infections. The foreskin façade provides under the commonly peeling off of epithelial cells and secretions from the glands provide an inviting warm, damp culture environment for organisms. Therefore, proper personal hygiene is very important in the prevention of balanoposthitis.
Other notable causes include:
- Usage of harsh soaps for genital wash
- Staphylococcus aureus infection
- Candida albicans infection
- Uncontrolled diabetes
- Improperly rinsing soap off during bathing
- Diseases like lichen sclerosis and reactive arthritis.
Balanoposthitis Diagnosis
For the diagnosis of this condition, physician will do a physical assessment, which will reveal the symptoms most commonly associated with balanoposthitis. Aside from physical examination, proper history is also taken. Other tests include:
- Laboratory studies
- Potassium hydroxide Test: This is done to check presence of candidial infections. This is also cultured to know the specific antifungal medication to which the organism is sensitive.
- Serologic Test: This test may be prescribed for candidial infections, especially in cases where the infection is unclear.
- Skin Biopsy: This procedure is done if the recommended antifungal therapy does not produce a good result. This is also done to check for the malignancy of the affected area and to rule out other conditions.
Balanoposthitis Treatment
The management and handling for this condition concentrates on clearing the onset of infection and inhibiting the periodic irritation or infection by way of enhanced hygiene.
The treatment regimen for balanoposthitis is also dependent on the cause. If the infection is caused by a bacteria, then treatment will antibiotics. Treatment may also include steroid based creams to reduce the inflammation.
Supportive Care: Proper personal hygiene and washing your hands regularly Exposure of the affected part to air will help stop the growth of anaerobic microorgasims.
Medical Care: Applying topical creams are the treatment that is widely used for this condition. The aim of this therapy is to eradicate the different microorganisms and to arrest inflammation.
Antifungal Therapy: The means by which this class of drugs act includes slowing down the conduits of substances essential for the production of the organisms’ cell membrane or changing the capacity of cell membrane to let substance pass through the cell membrane of the fungal cells.
Cotrimazole (Lotrimin, Fomisol 7, Mycelex, Gyne-Lotrimin): These are drugs with broad spectrum antifungal action. These are used to remedy infections of the skin, which results from different varieties of microorganisms causing skin disorders and yeasts. It slows down the growth of yeasts by changing the capacity of the cell membrane to let substance pass through, which results to demise of fungal cells. 1% cream is usually prescribed.
Antimicrobial Therapy: The mechanisms by which these drugs function tend to obliterate the microbes causing the infection, to arrest their reproduction or development, or to stop their illness causing actions.
Metronidazole (0.75% MetroGel Cream or lotion, 1% Noritate cream): This in imidazole with the capability to reduce the multiplication of anaerobic bacteris, protozoa, and fungi. It also provides an inflammatory effect, which involve inflection of white blood cells action.
Steroid Creams: This acts by inhibiting the inflammation of the glans penis and the foreskin.
Surgery: This is indicated in severe cases where the foreskin can no longer be retracted for cleaning. Circumcision is probably the best choice in treating this condition.
Balanoposthitis Prognosis
The expected outcome for balanoposthitis is high. Most patients who suffer from this condition have good prognosis since in most instances; the condition can be restricted with the use of specially medicated creams and with proper and improved personal hygiene. Circumcision is generally not needed especially if the balanoposthitis is not that severe and foreskin is still retractile and smegma can still be removed.
Complications
Normally, balanoposthitis do not exhibit any kind of complications especially if the patient has good compliance to treatment regimen. Again, early detection and treatment is very important. But, if the condition is left untreated or the inflammation or infection has been prolonged, it can lead to several complications such as:
- Scarring of the penis’
- Narrowing of the penile orifice, a condition known as meatal stricture
- Phimosis or severe tightening of the prepuce making it hard to bare the head of the penis
- Paraphimosis or the difficulty pushing the foreskin on top of the end of the penis
- Deacreased blood supply to the end of the penis as a result of the narrowed penile orifice
Prevention
The best prevention of Balanoposthitis and any other condition is having a proper and good hygiene. Being free from any kind of infections or disease all comes down to personal hygiene. Bathing regularly will help reduce the incidence of contracting balanoposthitis. During bath time, gently drag down the foreskin to reveal the end of the penis and clean it with water and soap. Remember to rinse off the soap properly and pat dry the part beneath it. Regular hand washing is also recommended to reduce the likely of infection. If you see changes around scrotal and penile areas, consult a doctor and avoid self diagnosis and self medication.
Balanoposthitis Pictures
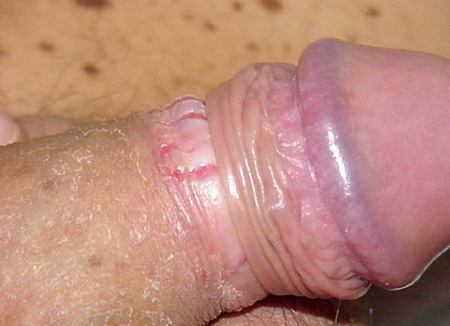
Picture 1 – Observe unretractility of the foreskin
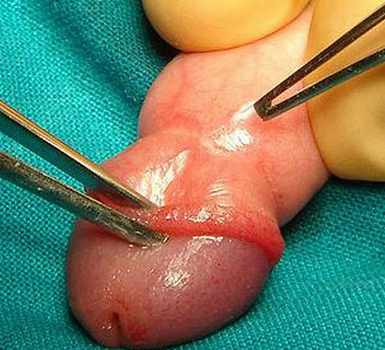
picture 2 – surgical procedure for Balanoposthitis