Blocked Tear Duct in Babies and Adults – Treatment, Symptoms, Pictures
What is Blocked Tear Duct?
When the small tubes or ducts that drain tears from the eyes are obstructed, the resulting condition is a blocked tear duct; this is also called as dacryostenosis.
The Anatomy of Tear Ducts
The tear duct or the nasolacrimal duct is a structure responsible for draining tears from the lacrimal gland or sac to the nasal cavity. This duct runs through the eyes and into the nasal cavity, it actually drains some of the excess tears into the inferior nasal meatus. This is the reason why crying is followed or accompanied by a runny nose.
The tear ducts have a small opening in the inner canthus of the eye (inner part of the eye), acquired obstructions can plug this opening and the drainage of the nasolacrimal ducts. Aside from that, congenital conditions, tumors and infections also contribute to a blocked tear duct.
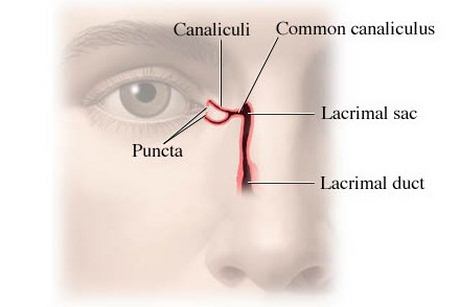
Image Source – Health.com
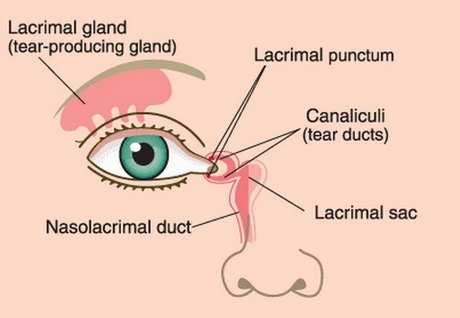
Picture 1,2 shows lacrimal duct, lacrimal glands and tear ducts
Blocked Tear Duct in Adults
Dacryostenosis is a common occurrence among newborns or pediatric clients. But the same condition can also affect adults. According to certain studies, almost 3% of clinical visits are due to problems of the nasolacrimal duct. In adults, probable causes of an obstruction of the tear ducts include the following:
- Chronic inflammation
- Fibrosis
- Neoplasms or malignant growths
- Infections
- Trauma
- Systemic diseases
Chronic Inflammation
Inflammatory processes can cause the tear ducts to be blocked. Chronic inflammation is more commonly seen in adults than in children. Such inflammation can be caused by other underlying diseases such as an autoimmune disease.
Fibrosis
Fibrosis formation is usually a result of chronic inflammation or infection. Fibrosis is the formation of fibrotic tissues, which are hard and alters the structure of the adjacent healthy tissues. Fibrous formations can be compared to scars. When scars form in the nasolacrimal duct (which is relatively small area), obstructions can occur.
Neoplasms or Malignant Growths
Malignant growths that obstruct the nasolacrimal gland are rare occurrences but is life threatening. Neoplasms or malignant tumors usually arise in the epithelial or mesenchymal layer of the lacrimal gland, where epithelial tumors account for almost 70% of the cases. Most malignancies affecting the nasolacrimal duct is a manifestation of another systemic condition.
Infections
Bacterial or fungal infections in the eye and nasolacrimal duct can also cause obstructions. Debris from the microorganism and the body cells that fight these organisms can block the small tubes and openings of the nasolacrimal drainage. Microorganisms such as Staphyloccoccus aureaus, Streptococcus, Chlamydia and even Helicobacter pylori are related to infectious obstructions of the tear duct.
Systemic Diseases
Systemic conditions such as sarcoidosis and Wegners granulomatosis can also be causes of bloked tear ducts. Systemic diseases are conditions that affect the whole body and not just a local organ or system. In both conditions, inflammatory cells or granulomas form in different parts of the body for unknown reasons.
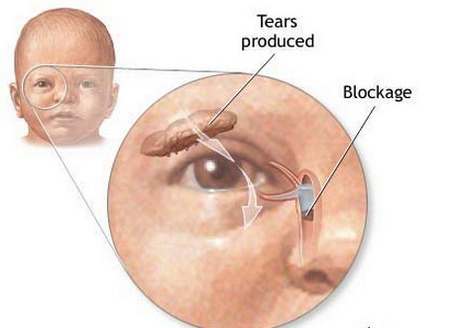
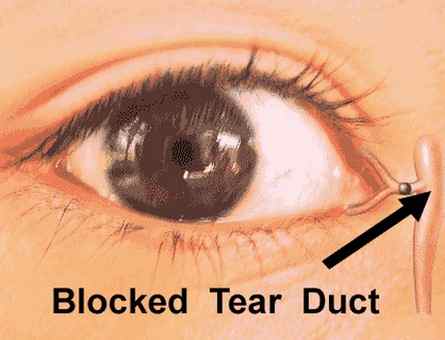
Picture 3, 4 shows blockage of tear duct system
Image Source – Medindia.net
Blocked Tear Ducts in Babies
Blocked tear ducts are most common among newborns and infants than in adults and it has the following causes:
- Congenital malformations
- Malformations of the skull and face
- Facial injuries
- Infections or inflammations
Congenital malformations
A blocked tear duct occurs in almost 6 out of 100 babies, or almost 20% among newborns in some studies. This occurs primarily due to the nasolacrimal duct that formed abnormally (begins inside the womb), or a tear duct that is not yet fully developed.
In most cases a flap of thin tissue covers the opening of the tear duct, as the new born grows and develops, the flap of tissue disappears and the opening becomes patent.
However, in certain conditions where the tear ducts fail to develop and remain blocked, medical treatment and surgery might be considered.
Malformations of the skull and face
An abnormally developed nasal bone can press onto the tear duct, closing if off and leading to an obstruction. Conditions where the nasal cavity and other structures of the face are malformed can also cause a blocked tear duct.
Infections or inflammations
Cellular debris from bacteria and white blood cells, as well as the swelling brought about by the inflammatory process can cramp up the nasolacrimal duct causing it to be obstructed.
Symptoms
- Wet teary eyes
- Excessive tearing or epiphora
- Redness of the eye
- Puffy eyes
- Pain or swelling of the lacrimal glands (found at the inner corner of the eye)
- Pus discharge from the eye or lacrimal gland
- Eyelid inflammation
- Vision changes
- Presence of cyst or tumor on the corner of the eye
- Asymmetrical eyes
- Unilateral exophthalmia or bulging of the eyes
- Presence of multiple granulomas surrounding the eye
Causes
- Congenital malformations
- Craniofacial abnormalities
- Chronic inflammation
- Infection
- Tumor growths or neoplasms
- Facial injuries or trauma
- Systemic conditions
Diagnosis
To diagnose a blocked tear duct, the following tests are done:
Dacryocystoshraphy
This is an eye imaging test where a contrast dye is utilized to evaluate the drainage of the nasolacrimal duct. The contrast dye is passed through the patient’s tear drainage system and a CT scan, MRI or an X-Ray is taken while the dye is inside the nasolacrimal duct to determine the cause of obstruction and its location.
Fluoresceine dye disappearance test
In this test a drop of a special dye is placed on the eyes. With a normal tear duct, some of the dye would be absorbed and drained by our tear ducts, but when a significant amount stays on your eye, it could indicate an obstruction.
Irrigation
This procedure simply involves irrigation of the eye with a saline solution to check if the ducts are draining properly.
Probing
A small, slender probe is inserted in the puncta (the small opening on the corner of the eye), to view the nasolacrimal duct and check for any obstructions.
Treatment
Treatment can be classified as Invasive and minimally invasive procedures
Minimally invasive procedures
Topical Antibiotics and Massage
This treatment regimen is particularly effective to younger age groups (1-12 months old) with blocked tear ducts. Proper massage can stimulate the drainage of the tear ducts and improve the child’s condition. In a study, almost 32% of the patients with blocked tear ducts improved with the two interventions alone.
Irrigation and Probing
The two procedures are usually done to diagnose the condition or figure out the cause of the obstruction. In certain cases (especially for pediatric patients), irrigation and probing can serve as the treatment for the condition. This may be due to the fact that the procedure dilates the puncta of the eye, which the relives the condition in most cases.
Use of Crawford Tubes
Insertion of tubes to dilate the nasolacrimal duct had been proven effective for children of all age groups. This treatment is a surgical treatment and is done if massage, antibiotics and probing failed to relieve the condition.
Invasive Treatment
External Dacryocystorhinostomy
This is a surgical procedure that involves the creation of a fistula of the lacrimal gland into the nasal cavity. This can alleviate the symptoms such as poor drainage and inflammation. This procedure was first done in 1911, but has failed due to unwanted side effects. But with the advances in medical and surgical technology, the procedure approaches a nearly 100% success rate.
Complications
When an obstructed tear duct is not treated, it could lead to the following complications:
- Recurrent infections
- Pain and discomfort brought about by the swelling
- Stagnant drainage
- Chronic inflammation
- Conjunctivitis
- Blepharitis
- Severe exophthalmia (in the case of tumor fomations)
Seek immediate Medical Attention if:
- There is a cyst, tumor or growth that is large or rapidly growing
- If the obstruction causes severe and persistent symptoms
- If the obstruction causes changes in the contour, shape and position of the eyes
- If other systemic symptoms are present, such as fever, pain, fatigue, and weakness
Prevention
Prevention primarily focuses on measures to avoid eye infection or inflammation. Other causes of blocked tear ducts such as congenital anomalies have no known prevnetions.
Prevent a blocked tear duct by employing the following measures:
- Avoid contact with people who have eye infections such as conjunctivitis
- Do not rub your eyes especially with bare hands or if your hands are not clean
- Proper hygiene and make up removal
- Keep contact lenses clean, use them properly and hygienically
- Wash your hand regularly