Myxedema Coma – Treatment, Symptoms, Causes, Diagnosis
What is Myxedema Coma?
Myxedema coma is a condition resulting from decompensated or unmanaged hypothyroidism. Hypothyroidism is the condition wherein the thyroid gland does not secrete adequate amount of thyroid hormones leading to problems in various metabolic processes in the body.
Myxedema coma present as a normal hypothyroidism based on laboratory tests, but other serious conditions can trigger the development of the state. The condition results from severe and persistent low thyroid hormones that cause loss of brain function. Myxedema is the most severe form of hypothyroidism and may result in death.
Myxedema coma is also considered a rare development of hypothyroidism. It is seen more in women and elderly patients with hypothyroidism. Myxedema coma is also increased during winter months because of increased cold intolerance experienced by patients.
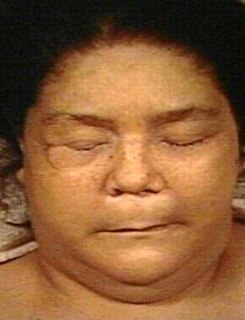
Myxedema Coma
Myxedema Coma Symptoms
Symptoms of myxedema coma result from the affectation of the brain as well as other organs in the body. Generally, the symptoms include slowing down of the functioning of the body. These include:
- Altered mental status – Patients often exhibit alteration in the level of consciousness that may start from disorientation to lethargy and eventually coma.
- Seizures – Seizures are a common manifestation of myxedema coma because of altered firing of nerve impulses in the brain.
- Anasarca or generalized edema – Poor metabolism of fats, proteins and carbohydrates leads to reduction in the osmotic pressure in the blood. The fluids tend to shift from the intravascular space into the interstitial space. Edema is often seen on the periorbital area and the tongue. Severe edema may involve the lungs and the heart membranes.
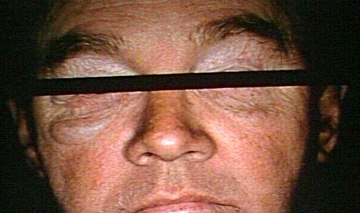
Anasarca as a symptom of Myxedema Coma
- Hypothermia – The core temperature of the body is often reduced up to 26.6 degrees Celsius. Patients initially have cold intolerance that progresses to severe loss of heat from the body.
- Hypotension – The cardiovascular integrity is also affected leading to a loss of vascular tone as a result of impaired heart contractility as well as loss of fluid in the blood vessels.
- Hypoglycemia – The reduction on the metabolic rate affects the conversion of carbohydrates into glucose leading to hypoglycemia.
- Bradycardia – The reduced metabolic rate also slows down the contraction of the heart muscles. Patients may suffer from cardiac arrest when not treated promptly.
- Hyponatremia – The increase in fluids in the body dilutes the blood and leads to hyponatremia or the low level of sodium.
- Hypoventilation – The respiratory system is also affected due to central nervous system depression.
Myxedema Coma Causes
Myxedema coma initially starts as hypothyroidism. Hypothyroidism may be caused by several factors such as radioactive exposure of the thyroid glands, overtreatment of hyperthyroidism, thyroid surgery or hypothalamic and pituitary problems, which leads to poor stimulation of the thyroid gland to produce hormones.
Myxedema coma is usually triggered by several factors, which increases the burden to the thyroid gland to produce more thyroid hormones. These include:
- Medications – Medication intake including anesthesia, narcotics, sedatives, lithium and amiodarone can trigger myxedema coma
- Infections – Infections increase the metabolic rate of the body, which the thyroid is unable to support.
- Trauma – Trauma also increases the demand for thyroid hormones in order to hasten healing.
- Hypothermia – The presence of a very low body temperature leads to severe cold intolerance that may affect the brain and the heart cells.
- Stroke – Stroke impedes the blood flow to the brain and may limit the functioning of the pituitary gland leading to further inactivation of the thyroid gland.
- Hypoglycemia – Hypoglycemia is also a trigger for myxedema coma because of poor oxygenation of the brain as a result of low blood sugar levels.
- Gastrointestinal hemorrhage – Hemorrhage may also lead to myxedema coma as a result of hypovolemia.
Myxedema Coma Pathophysiology
Myxedema coma usually develops when the patient’s homeostatic mechanisms are impaired as a result of various factors discussed earlier. The lack of equilibrium in the body intensifies the effect of hypothyroidism leading to brain affectation.
Myxedema Coma Diagnosis
The diagnosis of myxedema coma is made by testing for thyroid hormones and observing the symptoms. The presence of low thyroid hormones such as T3, T4 as well as TSH levels with the presence of the above symptoms are indicative of the condition. Other tests may be done such as blood tests and chest X-rays to determine sodium levels as well as edema of the lung and heart membranes. CPK levels are also checked using blood tests to determine altered permeability of the muscles.
Myxedema Coma Treatment
Treatment of myxedema coma usually involves emergency measures to reverse the condition and prevent death. Myxedema coma is highly fatal and patients usually die from cardiac and respiratory arrest. Patients are often placed in the intensive care unit for continuous monitoring and treatment. The first 48 hours is very critical in the treatment of myxedema coma in order to reduce mortality. Treatments include:
Intravenous Administration of Thyroid Hormones
The principal reason for myxedema coma is the reduction in thyroid hormone levels. In this regard, intravenous levothyroxine is usually employed to regain normal levels of thyroid hormones as fast as possible. Intravenous route is the choice because the gastrointestinal system is often compromised.
Antibiotic Therapy
Myxedema coma is usually preceded by an infection, thereby; bacterial etiology should be identified in order to give the most appropriate antibiotic treatment. Infections that usually result in myxedema coma is pneumonia and urosepsis.
Corticosteroids
Corticosteroids are usually administered to reduce cerebral edema as well as correct adrenal insufficiency because of hypopituitarism. Cortisol levels are initially taken to determine the level of glucocorticoids in the body. Hydrocortisone is given 5 to 10 mg per hour.
Respiratory Support
Mechanical ventilation is usually employed for patients with respiratory compromise (the presence of hypercapnia, hypoventilation and respiratory acidosis).
Rewarming
Patients also need passive rewarming with the use of warm environment and blankets. Rapid rewarding is contraindicated because of rebound effects.
Intravenous Infusion with Saline Solution
Hyponatremia requires infusion of saline to regain normal sodium levels and water regulation in the body. Intravenous infusions also correct hypovolemia.
Intravenous Glucose Administration
Glucose must also be administered to improve oxygenation of the brain cells as well as regain normal energy production.
These treatments should be given as soon as possible to prevent death. The prognosis is often undefined because of small number of incidences.