Spinal Muscular Atrophy – Symptoms, Pictures, Treatment and Life Expectancy
Spinal Muscular Atrophy is otherwise known as SMA, Hereditary Motor Neuropathy or Progressive Muscular Atrophy, is a cluster of autosomal-recessive disorders represented by advancing weakness and paralysis of the lower motor neurons. This disorder influences muscle contractions. This genetic disease damages the neurons which are found in the spine. These neurons work together with voluntary muscles in the arms and legs to elicit movements like creeping, ambulating, breathing, swallowing and movements of the neck and the head. With SMA, you lose all these abilities.
Genetics
In SMA, the child affected by SMA inherited two copies of faulty gene, one from each parent. While parents are not typically afflicted with SMA, each of them is carriers of one copy of the faulty gene.
How can you inherit SMA?
To acquire SMA, a person must inherit two SMN1 genes, one coming from each parent. Since the parents of a child afflicted with SMA have only one mutated SMN1 gene, they either do not show or express any signs and symptoms of SMA and do not have SMA. Therefore, one normal SNM1 gene is enough to compensate for the other faulty gene and can still function normally. This person is then called a carrier. Only 2% of the cases show that they are not carriers, but have SMA.
Types
Type I: Infantile
- Other name: Werdnig-Hoffmann Disease
- Onset: 0 – 6 months
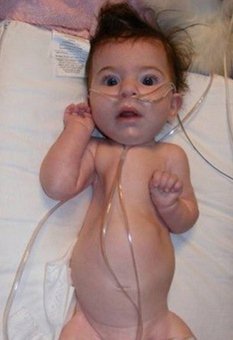
- Characteristics: This is a severe form of SMA that is represented by quick and unexpected onset, “floppy baby syndrome,” which manifests in the first months of life. The hasty death of these cells results in the inefficiency of major bodily organs and pneumonia-induced respiratory malfunction which is the most often cause of death.
- Life Expectancy: These babies do not commonly live past the age of two since death occurs as early as within weeks.
Type II: Intermediate
- Other name: Dubowitz Disease
- Onset: 6 – 18 months
- Characteristics: This type of the disorder commonly affects children who are never able to walk and stand but able to sustain a sitting position for at least some time in their life. Body muscles are weakened and respiratory system is of great concern.
- Life Expectancy: Reduced but most live well.
Type III: Juvenile
- Onset: more than 18 months
- Characteristics: This type is commonly describes a patient who can walk without support at some point, but later on lose the ability to walk.
- Life Expectancy: Normal to near normal
Type IV: Adult-onset
- Other name: N/A
- Onset: more than 35 years
- Characteristics: This type is also called late-onset SMA type III which usually appears with slow weakening of the muscles. Complications are uncommon.
- Life Expectancy: Normal
Signs and Symptoms
Here are the general signs and symptoms of SMA regardless of the type:
- Loss of muscle tone particularly on the extremities, rib, chest, and bulbar (facial) muscles
- Limpness or likeliness to drop or flop
- Loss of reflexes particularly in the extremities (areflexia)
- Struggling to attain developmental milestones
- Difficulty sitting, creeping and ambulating
- Imitating a frog-leg position upon sitting (hips abducted and flexed knees)
- Respiratory distress
- Bell-shaped torso due to the use of abdominal muscles only when breathing
- Poor feeding with great efforts in sucking and swallowing
- Twitching of the tongue
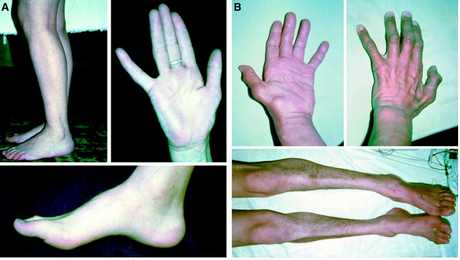
- Multiple congenital contractures (arthrogryposis)
Causes
The only noted cause of SMA is mutation of the protein composition of the gene which a plays a crucial part. The gene is faulty or mutated in such a way that it can no longer correctly and properly code the protein. This mutation is either caused by deletion that happens on exon seven or at other sites of aberration.
Diagnosis
The diagnosis of SMA includes careful history assessment and carefully performed neurologic examination. These methods will allow healthcare providers to extract the following:
- A family history of neuromuscular diseases
- Flaccid or floppy muscles
- Tongue muscles twitching upon physical assessment
- Absence of deep tendon reflexes
The following tests are also performed to confirm diagnosis:
- DNA testing (definitive test)
- Creatine kinase (CK) levels commonly normal in SMA type I or it is slightly increased in other types.
- Electromyography differentiates SMA from other neurogenic and myopathic diseases
- MRI of the spine will show cross section of the spine to detect motor neuron deficiency
- Muscle biopsy distinguishes SMA from other disorders of the neuromuscular system
Treatment
For spinal muscular atrophy, no treatment had been found effective especially in halting the progression of weakness caused by the disease. In this case, supportive care is very important. Treatment is usually centred on the respiratory system since patients are very prone to choking. Complications regarding breathing are also common.
The following are the major areas of concern:
- Respiratory Care: This requires the most attention since this area never recovers once weakened. Non-invasive ventilation is often used, and tracheotomy in more severe cases. These methods of ventilation increases survival rate in similar ways.
- Nutritional Care: Because of difficulties in swallowing, opening the mouth and chewing cause patient at risk for malnutrition.
- Orthopaedics: Development of kyphosis, scoliosis and other orthopaedic problems are more likely since spine muscles are weakened. Spine fusion is sometimes done in SMA type I and type II once patients reach the age of 8-10 to ease the pressure on the lungs. Physical and occupational therapy might also be beneficial to SMA patients.
- Mobility: Assistive devices will greatly help patients to move about and be independent in performing daily activities and will increase the quality of life.
- Cardiology: Even if the heart is not a great concern, SMA has been liked to some heart conditions.
- Mental health: SMA patients have reportedly high degree of contentment in life and their cognitive development are slightly faster than those not suffering from SMA and in certain degrees pose above-average intelligence.
Emerging therapies for SMA aims to correct the defective or mutated gene and to restore SNM levels to revert the symptoms.
- Gene therapy
- Stem Cell Therapy
- SNM2 Activation
- SNM2 Alternative Splicing Modulation
- SNM Stabilization
- Neuroprotection
Life Expectancy
Patients affected with SMA generally get worse over time, but the life expectancy and prognosis differs or depends on the type of SMA the patient have.
- Type I SMA has the shortest lifespan since it is the most severe type of the disorder. Although milder cases of Type I can live well until adulthood.
- The lifespan of a patients affected with Type II SMA is reduced compared to that of a healthy person. They can still become parents and grandparents.
- Type III SMA affected patients live longer with a life expectancy of nearly normal to normal.
- Adult-onset SMA (Type IV) patients can live as normal as possible and their deformities or mobility impairment does not affect their life expectancy.
Pictures